Menu
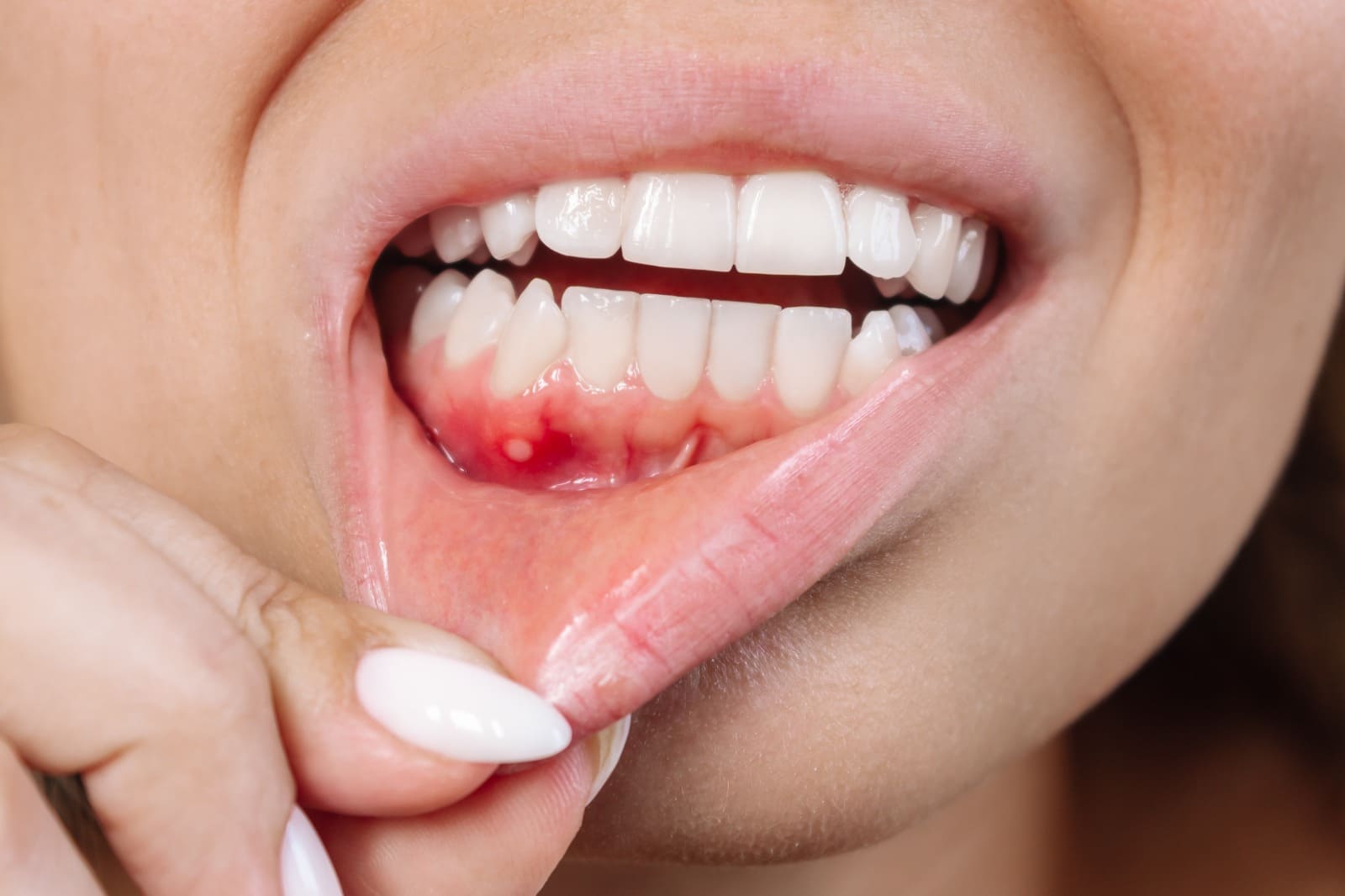
When a patient presents with fiery red, peeling, and intensely painful gums, our clinical reflex is almost automatic: reinforce oral hygiene, prescribe an antimicrobial rinse, and schedule a follow-up. But what happens when the tissue simply refuses to heal?
According to the 2017 Classification of Periodontal and Peri-Implant Diseases, non–plaque–induced gingivitis encompasses a complex group of conditions. Clinically, these frequently present as “desquamative gingivitis” (DG) a descriptive term for the shedding of the gingival epithelium that often masks underlying autoimmune mucocutaneous disorders like Oral Lichen Planus (OLP) or Mucous Membrane Pemphigoid.
A recent observational study evaluated just how long it takes for these specific patients to get an accurate diagnosis. The results expose a massive blind spot in general practice.
The study tracked 86 patients presenting with desquamative gingivitis at specialized oral medicine centers. The most striking statistic was the timeline: the mean diagnostic delay was a staggering 10 months.
That is nearly a year of patients enduring burning oral pain, undergoing painful mechanical debridement, and cycling through ineffective topical treatments before finally receiving a definitive autoimmune diagnosis.
To understand how to fix this, the researchers analyzed the associated factors. The data revealed several nuances that challenge our daily clinical assumptions:
The study explicitly noted that smoking habits had no impact on the diagnostic delay. When tissues don’t heal, it is easy to blame the patient’s smoking habit. This data reminds us that we cannot use smoking as a clinical excuse to ignore non-responsive, sloughing tissues.
Diagnostic delay was significantly higher for patients attending private oral health centers (11.19 months) compared to public centers (8.75 months; $p < 0.05$) . Why? It is highly likely that general dentists in the private sector attempt prolonged “trial and error” management—changing mouthwashes, re-scaling, and “watching”—before finally referring the patient to a private oral medicine specialist. Furthermore, geographic distance from a diagnostic center also significantly increased the delay.
Desquamative gingivitis is not a final diagnosis; it is a glaring clinical warning sign.
The takeaway protocol: If a patient presents with fiery, sloughing gingiva that does not respond to standard mechanical debridement and strict plaque control within 2 to 4 weeks, you must pivot. Do not prescribe another round of chlorhexidine. It is time to refer to a specialist or perform a biopsy. Breaking the 10-month cycle of delay starts with recognizing when plaque is no longer the enemy.
Caggiula A, Romano F, Dentico E, Pinto F, Lopez-Jornet MP, Petruzzi M. Diagnostic Delay in Desquamative Gingivitis: An Observational Cohort Study. Oral Dis. 2026 Mar 19. doi: 10.1111/odi.70276. Epub ahead of print. PMID 41853924.


| PRODUCTS | QTY | PRICE | VALUE in INR |
|---|
| PRODUCTS | QTY | PRICE | VALUE in INR |
|---|